Immunogenicity remains a central consideration in biopharmaceutical development, even as biologics and advanced therapies continue to expand across therapeutic areas. Its impact extends beyond safety, influencing efficacy, dosing durability, and long-term treatment outcomes.
From a strategic perspective, proactive immunogenicity management supports patient-centric development, reduces late-stage clinical risk, and enables broader market access. This is especially important for chronic therapies and globally deployed biologics where variability in patient populations and treatment conditions can amplify immune response risks.
This blog examines immunogenicity in biopharmaceuticals across the development lifecycle, highlighting key mechanisms, influencing factors, and regulatory expectations, along with practical approaches to assess and manage immunogenicity risk effectively.
Key Takeaways:
- Immunogenicity directly affects safety, efficacy, and regulatory success of biopharmaceuticals and must be managed across the entire development lifecycle.
- Unintended immune responses in therapeutic proteins and biologics can lead to ADA formation, reduced efficacy, and adverse clinical outcomes, while controlled immunogenicity is essential for vaccines.
- Early risk assessment, formulation design, and process control are key to minimizing immunogenicity-related failures in late-stage development and post-approval use.
- Regulatory expectations require validated assays and clinically meaningful interpretation of immunogenicity data across populations and regions.
- DRK Research Solutions supports end-to-end immunogenicity management through integrated development, GMP manufacturing, analytical support, and regulatory-aligned documentation.
What Is Immunogenicity in Biopharmaceuticals?
Immunogenicity is the ability of a biopharmaceutical product to provoke an adaptive immune response in the human body. In therapeutic settings, this often appears as the formation of anti-drug antibodies (ADAs), which can reduce or neutralise the drug’s activity, modify its pharmacokinetics, or cause adverse immune reactions.
Biopharmaceuticals are particularly prone to immunogenicity because they are typically protein-based and produced through complex biotechnological processes. Even minor differences in protein structure, formulation components, or impurities can significantly influence how the immune system recognises the product.
For developers, immunogenicity is a critical CMC and clinical risk parameter that directly influences formulation design, process controls, comparability strategies, and regulatory acceptability.
Why Is Immunogenicity a Key Consideration in Biopharmaceutical Development?
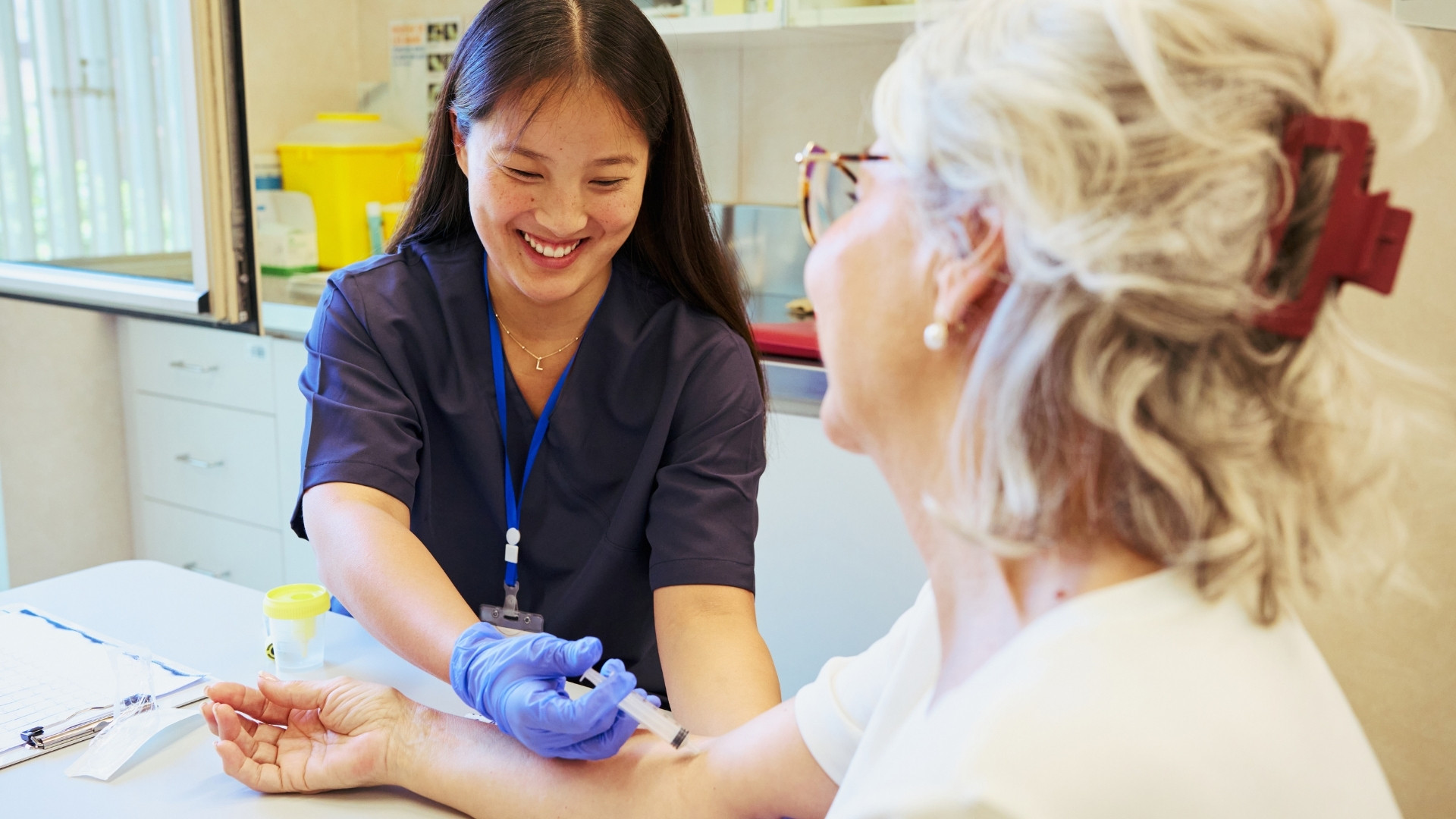
Immunogenicity assessment is a continuous process that spans the entire biopharmaceutical development lifecycle. Early predictive evaluation guides candidate selection and formulation decisions, while clinical-phase monitoring determines long-term safety, efficacy, and regulatory acceptability.
When immunogenicity is not addressed proactively, programmes risk late-stage clinical delays, post-approval safety concerns, and restrictive product labeling. For labelling therapies intended for global use, particularly in underserved populations, robust immunogenicity control is essential to maintaining regulatory confidence and sustained patient access.
Key focus areas across development include:
- Early-Stage Risk Prediction: Supports informed molecule selection and reduces downstream development risk.
- Formulation and Process Strategy: Helps control factors that influence immune response, such as impurities and aggregation.
- Clinical Monitoring and Interpretation: Clinical-phase immunogenicity monitoring informs long-term safety, efficacy, and regulatory acceptability, with development partners supporting data quality, consistency, and regulatory documentation.
- Regulatory Alignment: Ensures immunogenicity data meet global expectations for approval and inspection readiness.
- Global Deployment Considerations: Maintains consistency across populations, regions, and long-term use scenarios.
This lifecycle-based approach positions immunogenicity as a strategic development variable rather than a late-stage compliance requirement.
Desired vs. Undesired Immunogenicity: Key Comparison
In biopharmaceutical development, immunogenicity is primarily assessed as a risk factor for therapeutic proteins and biologics, where unintended immune responses can compromise efficacy, safety, or long-term treatment viability.
The table below highlights the key differences between desired and undesired immunogenicity, helping to clarify their clinical and regulatory implications:
| Aspect | Desired Immunogenicity | Undesired Immunogenicity |
| Purpose | Intentional induction of immune response (e.g., vaccines) | Unintended immune response to therapeutics (e.g., biologics, niche products) |
| Target | Protective immunity against a disease | Therapeutic protein or drug immunization molecule |
| Outcome | Controlled and beneficial; enhances health | Potentially harmful; may reduce efficacy or cause adverse reactions |
| Response Characteristics | Measured magnitude and durability indicate success | Can be variable, unpredictable, and persistent |
| Clinical Implications | Long-term disease prevention,
effective im |
ADA formation, hypersensitivity, altered dosing, treatment discontinuation |
| Regulatory Focus | Monitoring effectiveness and safety | Mitigation of risk and compliance with safety guidelines, particularly for chronic therapies |
| Management Approach | Optimised to achieve the desired immune activation | Minimised through formulation, process control, and clinical monitoring |
Understanding these differences allows developers and regulators to manage immunogenicity strategically, maximising beneficial responses while minimising potential risks.
Core Mechanisms Driving Immunogenicity in Biopharmaceuticals
Immunogenicity in biopharmaceuticals arises through well-defined biological pathways that determine the magnitude, durability, and clinical consequences of immune responses.
Identifying the likely immunogenicity mechanisms supports risk-informed formulation, manufacturing, and clinical monitoring strategies, particularly during comparability assessments and lifecycle changes.
1. T-Cell–Dependent Immunogenicity
T-cell–dependent responses occur when therapeutic proteins are processed by antigen-presenting cells and displayed via major histocompatibility complex (MHC) molecules, triggering helper T-cell activation.
This pathway typically leads to high-affinity, class-switched antibody production and long-term immunological memory. From a development standpoint, these responses pose the greatest risk due to their persistence and their potential to cause irreversible loss of therapeutic efficacy or altered safety profiles.
2. T-Cell–Independent Immunogenicity
T-cell–independent immunogenicity results from direct B-cell activation by repetitive or highly ordered antigen structures, without T-cell involvement.
Although these immune responses are often shorter in duration, they can still produce clinically relevant antibodies, particularly with chronic dosing, high exposure levels, or repeated administration.
A clear understanding of which mechanism predominates enables targeted risk mitigation, supports rational clinical monitoring strategies, and strengthens regulatory justification throughout the product lifecycle.
Methods for Measuring Immunogenicity
Understanding immunogenicity requires more than a single test. Regulatory expectations and clinical relevance demand a structured, tiered approach that combines multiple assay types to detect, characterise, and interpret immune responses across development stages.
Together, these methods generate robust, submission-ready immunogenicity data.
- Screening and Confirmatory Assays (ELISA and ECL): Screening and confirmatory assays, such as ELISA and electrochemiluminescence (ECL) are used to detect anti-drug antibodies (ADAs) with high sensitivity. These assays help identify immune responses early and confirm their specificity.
- Neutralising Antibody Assays: Neutralising antibody assays assess whether antibodies interfere with the drug’s biological activity, providing insight into the potential impact on efficacy.
- Cell-Based and Flow Cytometry Assays: Cell-based assays may be applied in select development programs to support functional interpretation of immune responses, with development partners ensuring assay validation, data integrity, and regulatory alignment.
- In Silico and In Vitro Risk Assessment Tools: In silico and in vitro tools support early immunogenicity risk assessment by identifying potential immunogenic epitopes before clinical exposure.
14 Key Factors That Influence Immunogenicity Risk
Immunogenicity results from the complex interaction of patient characteristics, treatment design, and product-specific attributes. Understanding these contributors helps guide formulation strategies, clinical monitoring, and regulatory risk management.
- Patient Genetics and Immune Status: Variations in HLA types, immune function, age, and comorbidities affect individual immune responses.
- Disease Profile: Underlying conditions, inflammation, and immune system dysregulation can enhance or suppress antibody formation.
- Prior Biologic Exposure: Previous treatments with similar proteins or vaccines may prime the immune system and increase risk.
- Route of Administration: Intravenous, subcutaneous, or intramuscular delivery each carries a different potential for immune activation.
- Dosing Schedule: Frequency, dose size, and treatment duration influence the likelihood of antibody development.
- Concomitant Medications: Co-administered therapies, including immunosuppressants, can alter immune response.
- Protein Sequence and Structure: Amino acid variations, sequence differences, or neoepitopes can trigger immune recognition.
- Aggregation and Stability: Protein aggregation, unfolding, or degradation products may increase immune responses.
- Post-Translational Modifications (PTMs): Glycosylation, pegylation, or other modifications can modify immunogenicity.
- Formulation Components: Buffers, stabilisers, and excipients can influence protein presentation to the immune system.
- Manufacturing Consistency: Batch-to-batch variability or process changes can affect immunogenic potential.
- Container and Storage Conditions: Interactions with packaging materials, leachables, or temperature variations can alter protein stability.
- Delivery Device: Needles, syringes, or auto-injectors may affect protein shear stress and immune response.
- Environmental Factors: Population and regional factors, including endemic disease burden and treatment conditions, may contribute to variability in observed immunogenicity rates and should be considered during global development and post-approval monitoring.
By considering these factors collectively, developers can design safer, more consistent biologics, anticipate immune responses, and ensure regulatory compliance throughout the product lifecycle.
How To Meet Regulatory Expectations for Immunogenicity Assessment?
Immunogenicity assessment is a core regulatory requirement for biologics, niche products, and certain advanced therapies. From a CMC perspective, regulators expect immunogenicity data to be supported by robust process control, comparability justification, and stability data that demonstrate consistent product quality across batches and lifecycle changes.
| Regulatory Focus | Key Action | Outcome |
| ADA Detection and Monitoring | Implement validated screening and confirmatory assays throughout clinical trials. | Enables reliable detection of immune responses and supports regulatory compliance. |
| Clinical Relevance Assessment | Evaluate the impact of ADAs on safety, efficacy, and pharmacokinetics. | Demonstrates whether immune responses affect clinical outcomes. |
| Neutralising Antibody Evaluation | Conduct neutralising antibody assays where applicable. | Assesses functional impact on drug activity and therapeutic performance. |
| Assay Validation and Sensitivity | Justify assay sensitivity, specificity, and cut-point determination. | Ensures data reliability and inspection readiness. |
| Population and Regional Consistency | Analyse immunogenicity data across patient groups and regions. | Supports global submissions and reduces regulatory risk. |
| Risk Mitigation Strategy | Define and document immunogenicity risk management approaches. | Strengthens regulatory confidence and long-term product viability. |
Meeting regulatory expectations for immunogenicity requires a coordinated strategy that integrates robust assays, clinically meaningful interpretation, and consistent documentation across development programmes.
How DRK Research Solutions Helps Manage Immunogenicity Risks in Biopharmaceuticals?
DRK Research Solutions supports biopharmaceutical developers by strengthening formulation robustness, manufacturing consistency, analytical readiness, and regulatory documentation that underpin effective immunogenicity risk control
- Early Immunogenicity Risk Assessment: Identifies potential immunogenicity risks during early development, enabling informed design, formulation, and process decisions before clinical progression.
- Formulation and Process Optimisation: Optimises formulations and manufacturing processes to reduce aggregation, instability, and impurities that can contribute to immune responses.
- GMP Manufacturing Through Qualified EU-Approved Facilities: DRK works with EU-approved manufacturing facilities in Europe and Asia to ensure consistent, GMP-compliant production supported by robust quality systems. This partnership model minimises variability and maintains product integrity across clinical and commercial supply.
- Immunogenicity-Focused Analytical and Stability Support: Provides analytical and stability data that support immunogenicity risk evaluation, comparability, and long-term product performance.
- Regulatory Documentation and eCTD Support: Prepares regulatory-aligned, eCTD-ready documentation supporting immunogenicity assessments and global submission requirements.
- Scalable Support from Clinical to Commercial Manufacturing: Offers flexible, scalable support for clinical trials and commercial production while maintaining consistent immunogenicity risk control.
- Drug Product Focus with Qualified API Sourcing: DRK supports drug product development and manufacturing while sourcing APIs/drug substances through qualified suppliers and approved vendor partners. This ensures regulatory compliance, supply reliability, and consistent downstream quality control.
Conclusion
Immunogenicity plays a decisive role in the safety, efficacy, and regulatory success of biopharmaceutical products. It influences clinical outcomes, long-term treatment reliability, and global acceptance, making it a core consideration throughout the development lifecycle.
Partnering with an experienced CDMO like DRK Research Solutions enables developers to address immunogenicity risks early through disciplined formulation development, controlled manufacturing, and regulatory-aligned documentation, reducing uncertainty across clinical and commercial stages. Connect with us to explore how integrated immunogenicity management can support your program from early development through commercialisation.
FAQs
1. What is immunogenicity in biopharmaceuticals, and why is it important?
Immunogenicity is the ability of a biopharmaceutical, such as a biologic or biosimilar, to trigger an immune response in the body. It is important because unwanted immune reactions can reduce drug effectiveness, affect safety, and influence regulatory approval and long-term clinical use.
2. How does immunogenicity impact the safety and efficacy of biologic drugs?
Immune responses can lead to the formation of anti-drug antibodies that reduce a drug’s activity or increase its clearance from the body. In some cases, immunogenicity can also cause adverse reactions, making it a key consideration during development and treatment.
3. What factors contribute to immunogenicity in biopharmaceutical products?
Immunogenicity is influenced by factors such as molecular structure, formulation, impurities, manufacturing consistency, and route of administration. Patient-related factors, including genetics and disease state, can also affect immune responses.
4. How is immunogenicity evaluated during drug development?
Immunogenicity is assessed through laboratory assays, preclinical studies, and clinical testing to detect and characterize anti-drug antibodies. Ongoing monitoring helps teams understand the clinical relevance of immune responses and manage risks early.
5. How can immunogenicity risks be minimized in biopharmaceutical development?
Risks can be minimized through careful molecular design, stable formulations, strict control of impurities, and consistent manufacturing processes. Early assessment and continuous monitoring across development stages also play a critical role.
