Sterile injectable manufacturing is the most demanding segment of the pharmaceutical industry. These drugs enter the bloodstream directly, making sterility, particulate control, and pyrogen elimination regulatory imperatives rather than optional objectives.
For sponsors scaling clinical supply or preparing commercial launch, success requires a CDMO partner who can maintain process integrity, regulatory visibility, and continuity across global markets.
With growing demand for biologics, vaccines, and specialty injectables, robust sterile injectable manufacturing has become a core capability for advanced CDMOs.
This article outlines what sterile injectable manufacturing involves, why it is strategically critical, and how DRK Research Solutions supports development, tech transfer, and GMP production.
Key Takeaways:
- Sterile injectable manufacturing requires strict sterility, particulate control, and pyrogen elimination to meet regulatory standards and ensure patient safety.
- Success depends on a CDMO model that integrates aseptic formulation, technology transfer, and fill–finish execution under globally aligned quality systems, while using EU-qualified partners to ensure regulatory compliance, affordability, and supply continuity.
- Key operational risks include human intervention, fill-finish precision, equipment qualification, and handling sensitive biologics.
- Robust QC and QA, including endotoxin testing, CPP/CQA monitoring, and environmental oversight, ensure reproducible sterility and regulatory defensibility.
- Modern strategies such as isolator-led processing, single-use systems, inline inspection, and modular facilities improve process control and supply continuity.
Understanding Sterile Injectable Manufacturing: What Leaders Must Evaluate
Sterile injectables encompass drug products such as solutions, suspensions, emulsions, and lyophilized powders that bypass first-pass metabolism to deliver therapeutic action directly.
Common administration routes include intravenous (IV), intramuscular (IM), subcutaneous (SC), and intrathecal delivery. Unlike non-sterile formulations, sterile injectables have virtually zero tolerance for contamination due to the high patient safety and regulatory stakes.
For senior pharmaceutical and biotech decision-makers evaluating manufacturing partners, the critical question is not merely whether aseptic filling can be executed, but whether sterility assurance, documentation integrity, and regulatory oversight can be sustained consistently across internal teams, partner facilities, and global supply chains.
The focus is:
- Can they sustain sterility assurance across every batch?
- Can they defend processes and outcomes under regulatory inspection?
- Can they maintain continuity and compliance across global commercial supply chains?
This perspective shifts the evaluation from operational capability to strategic sterility governance, emphasising risk mitigation, regulatory readiness, and global supply reliability.
12 Ways Sterility Drives Compliance and Patient Safety in Injectables
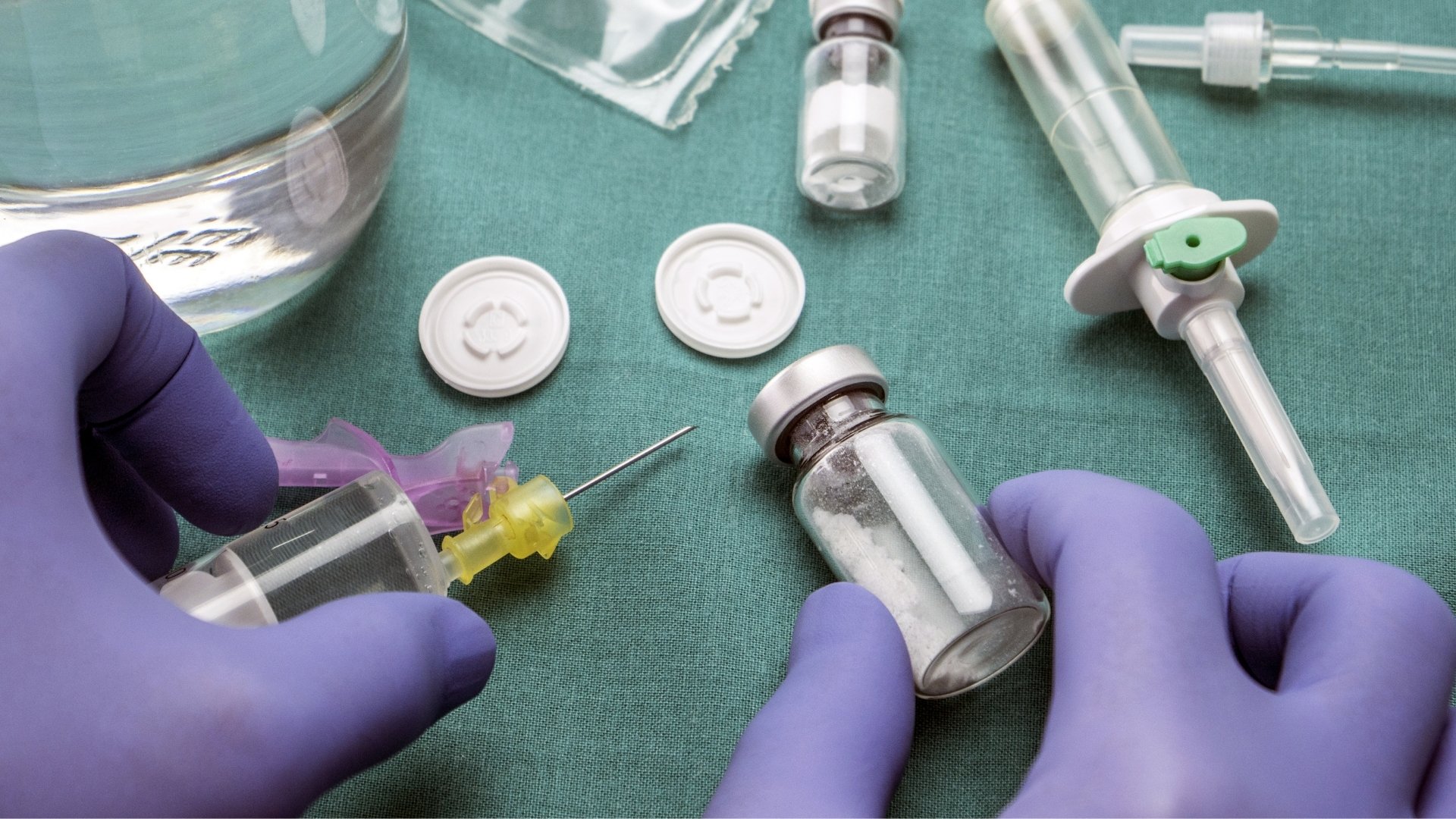
Ensuring sterility requires more than equipment or documented procedures. Regulatory agencies such as the FDA, EMA, MHRA, and WHO evaluate the maturity and defensibility of the entire system.
Critical considerations include:
1. Environmental Control & Cleanroom Compliance: Maintaining ISO-classified spaces, monitoring airflow integrity, and enforcing pressure cascades to prevent contamination.
2. Aseptic behaviour Evidence: Demonstrating operator adherence, minimal intervention, and process consistency rather than simply referencing SOPs.
3. Sterilization Validation: Validating terminal and in-process sterilization using D-values, sterility assurance level (SAL) targets, and load mapping to ensure predictable microbial kill.
4. Data Integrity & Traceability: Capturing complete batch records, deviations, media fills, and CAPA workflows to provide a defensible audit trail.
5. System Readiness over Equipment: Regulatory assessment focuses on contamination control strategies, monitoring systems, and procedural robustness regardless of whether operations are executed in-house or through qualified partner facilities under validated oversight models.
6. Container-Closure Integrity (CCI): Ensuring packaging integrity to prevent contamination during storage, transport, and administration.
7. Media Fill Simulation & Intervention Analysis: Using predictive media fill programmes to model worst-case operator interventions and environmental risk points.
8. Critical Process Parameters (CPPs) & Quality Attributes (CQAs): Continuous monitoring and control of parameters that influence sterility, product quality, and batch release decisions.
9. Risk-Based Preventive Maintenance: Scheduled validation and upkeep of HVAC, sterilisers, and isolators to prevent failures before they impact production.
10. Endotoxin & Particulate Control: Routine BET/LAL testing and particle monitoring to maintain patient safety and regulatory alignment.
11. Training & Qualification Programmes: Continuous operator training in aseptic technique and contamination prevention to reduce human-factor risk.
12. Audit Readiness & Regulatory Alignment: Documentation and monitoring systems designed for proactive inspections rather than reactive remediation.
A modern CDMO must integrate these elements into a cohesive, auditable framework. Only then can sterility become a predictable, verifiable component of injectable manufacturing, enabling regulatory confidence, clinical continuity, and reliable global supply.
6 Key Domains Driving Excellence in Sterile Injectable Manufacturing
The critical domains in sterile injectable programmes extend beyond traditional aseptic operations. They encompass technical precision, facility integrity, analytical rigor, and supply chain control. Understanding these areas helps leadership teams make informed, risk-aware decisions when selecting a partner for complex, high-value injectables.
| Domain | Executive Evaluation Lens |
| Aseptic Manufacturing | Minimisation of operator interventions, verification of airflow integrity, and mitigation of human-factor contamination risks |
| Terminal Sterilization | Validation of sterility assurance level (SAL), precise thermal profile mapping, and assessment of thermal or chemical impact on finished drug product stability. |
| Fill-Finish Operations | Defensible container-closure integrity (CCI) testing, line clearance verification, and media fill programmes aligned with regulatory expectations |
| Cleanroom Architecture | ISO classification adherence, maintenance of pressure cascade continuity, continuous environmental monitoring, and real-time analytics for intervention alerts |
| Analytical & QC Readiness | Alignment of critical quality attributes (CQAs) and critical process parameters (CPPs) with validated analytical methods for batch release and regulatory submission |
| Supply Chain & Materials Management | Controlled raw material handling, validated transport and storage conditions, and supplier qualification to ensure consistency and minimise contamination risks |
Each domain is interdependent. Any lapse can compromise sterility, regulatory compliance, or patient safety. A modern CDMO demonstrates integrated governance, process defensibility, and continuous monitoring across these domains whether execution occurs within internal facilities or through qualified manufacturing partners operating under unified quality and regulatory frameworks.
What Compliance Requirements Are Critical for Sterile Injectable Production?
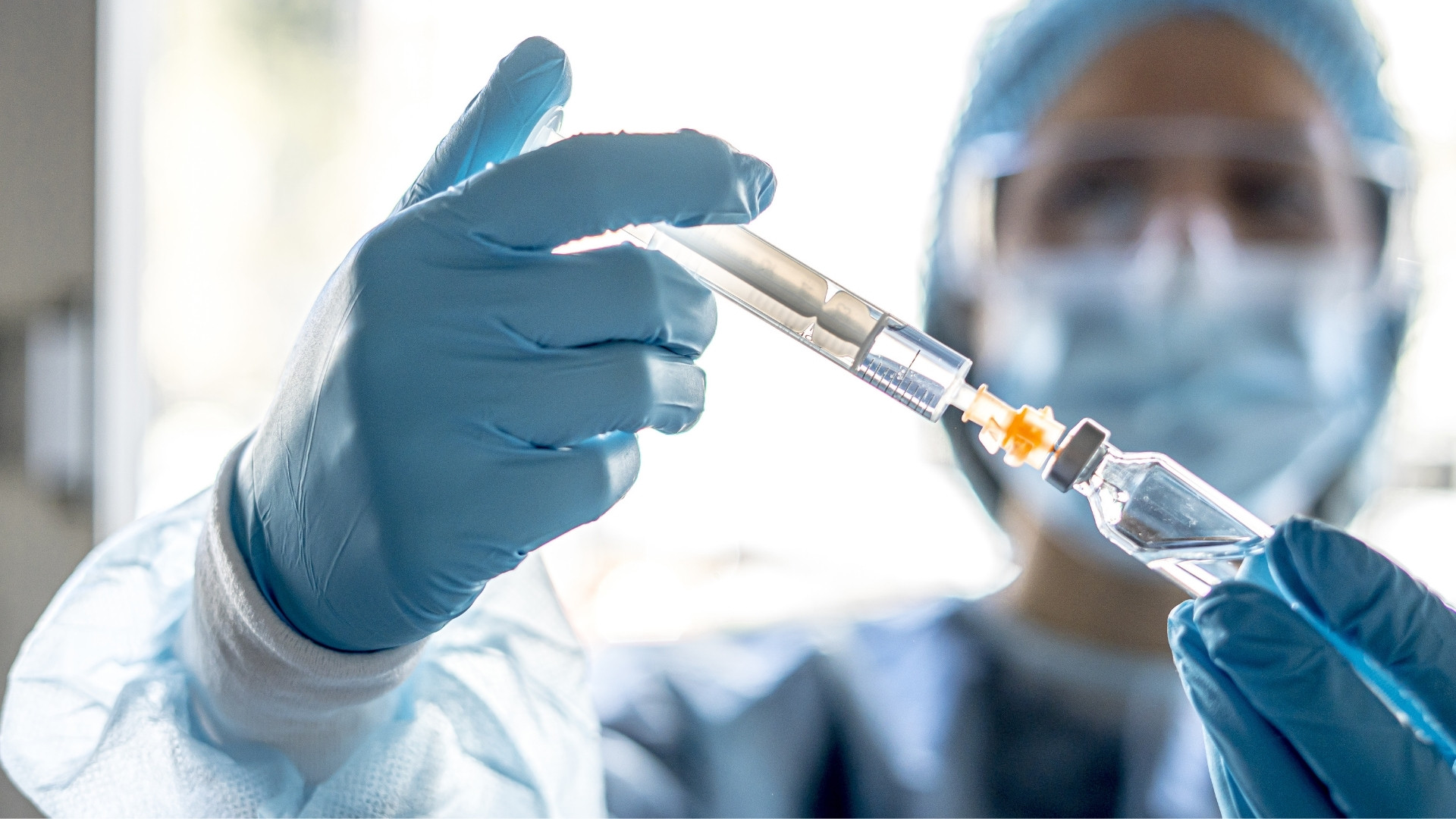
Compliance in sterile injectable manufacturing is not just a regulatory requirement. It is a strategic necessity that ensures product safety, protects market access, and reduces inspection and approval risks, especially for complex biologics.
Key regulatory anchors include:
- FDA 21 CFR Parts 210/211: Ensures cGMP compliance in drug production and quality control.
- EU GMP Annexe 1: Sets aseptic processing expectations, emphasising contamination control and process validation.
- WHO TRS 1025 and related guidance: Supports global market supply, reinforcing product safety in diverse geographies.
Check these inspection focus areas, which are evolving:
- Data integrity by design: Systems must prevent errors proactively rather than rely on audit remediation.
- Media fill programmes: Designed around realistic intervention probability, not demonstration cycles.
- Critical Container Closure Integrity (CCI) testing: Treated as a release-critical decision point, not optional QA documentation.
- Parametric Release Justification: Where applicable and regulator-approved, terminal sterilization processes may support parametric release strategies. These approaches must be product-specific, fully validated, and aligned with regional regulatory expectations.
A leading CDMO demonstrates regulatory readiness through reproducible processes, validated data, and inspection-defensible protocols rather than only showing intent.
Top 4 Critical Operational Risks in Sterile Injectable Manufacturing
Sterile manufacturing challenges are not merely operational issues; they directly impact regulatory approval, product integrity, and patient safety. To manage these effectively, organisations must identify the most critical risk areas and implement mitigation strategies that are both traceable and defensible under inspection.
Key operational vulnerabilities include the following:
| Challenge | Why It Matters | Risk If Mishandled |
| Human interaction in aseptic zones | Primary vector for microbial contamination | CAPA escalation, import holds, audit findings |
| Fill-finish precision | Determines dose accuracy, safety, and release compliance | Batch rejection, line stoppage, product recalls |
| High-sensitivity formulations (biologics, HPAPI drug products) | Thermally or chemically fragile active components are prone to degradation. | Loss of potency, assay failure, clinical inconsistency |
| Equipment qualification (HVAC, isolators, sterilisers) | Ensures consistent environmental control and sterility assurance | Regulatory non-compliance findings, delays in product approval |
Every mitigation plan must be inspectable and actionable, demonstrating control, traceability, and risk management rather than simply describing processes.
How Do Advanced QC and QA Strategies Strengthen Sterile Injectable Programmes?
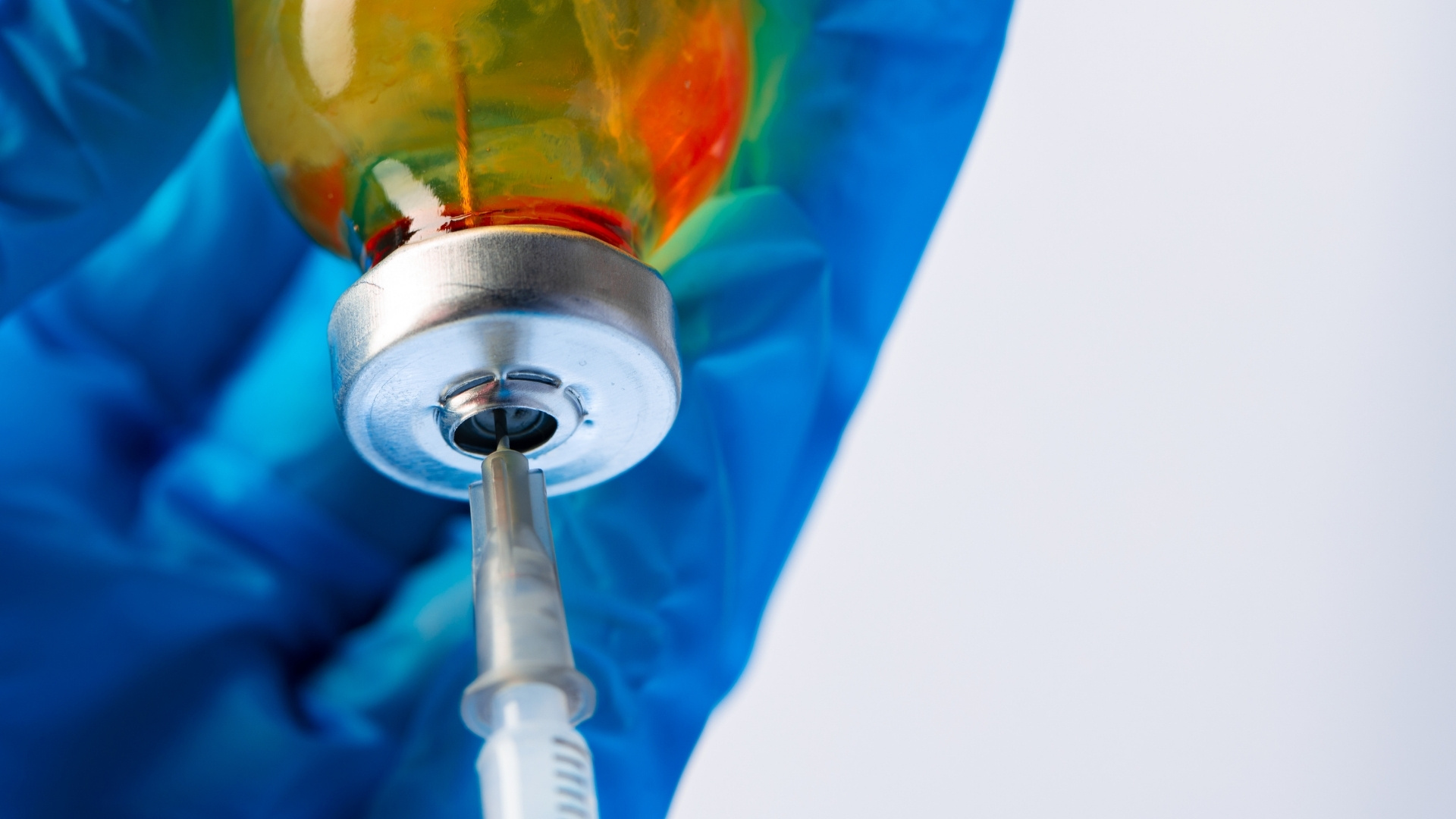
In sterile injectable programmes, quality is not just about meeting specifications. It is about demonstrating a controlled, reproducible system that maintains sterility consistently across development, scale-up, and commercial supply. QC validates the product while QA validates the system that ensures product quality.
Here are some key pillars of QC and QA execution:
- Sterility and Endotoxin Validation: Rigorous sterility testing, including bacterial endotoxin testing (BET/LAL), ensures that each batch meets pharmacopeial standards. QC data are integrated with QA oversight to prevent deviations from compromising sterility.
- Environmental and Event Monitoring: Environmental monitoring is tied to intervention logs and cleanroom activity. Traceable records of contamination risk enable trend analysis to inform process adjustments and maintain GMP compliance.
- In-Process Controls Aligned to CPPs and CQAs: Real-time monitoring of critical process parameters (CPPs) and critical quality attributes (CQAs) helps catch process deviations early. This prevents downstream batch rejection or rework.
- Operator Competency and Controlled Intervention: Sterile operations rely on highly qualified technicians trained to operate in low-tolerance environments. Interventions are planned, documented, and executed without compromising aseptic conditions.
- Predictable System Demonstration: A partner’s capability is measured by their ability to reproducibly demonstrate control of processes, environmental conditions, and personnel interventions across multiple batches and facilities.
Outcome for Sponsors:
Focusing on these pillars enables CDMOs to deliver sterile injectables with predictable quality, reduced regulatory risk, and a reliable path from early development to global commercial supply.
How Can Modern CDMO Execution Transform Sterile Injectable Programmes?
Modern sterile injectable drug product manufacturing demands more than cleanrooms and compliant equipment. It requires coordinated execution across formulation, aseptic processing, fill–finish, and regulatory alignment to ensure products stay stable, safe, and supply-ready. Sponsors are now prioritising CDMOs that can manage these variables as a unified lifecycle rather than as disconnected service steps.
Here’s where modern sterile systems are heading:
1. Isolator-Led Fill-Finish
Isolator systems increasingly replace RABS-dependent workflows to reduce manual interventions, improve sterility assurance levels, and align with future inspection expectations from EU and US regulators. This shift reflects a recognition that personnel exposure is the highest contamination vector, not equipment failure.
2. Single-Use and Disposable Flow Paths
The rising validation burden and the overhead of cleaning verification across multiple product lines drive the adoption of single-use assemblies. These systems shorten changeover windows, reduce cross-contamination risk, and suit contract teams managing hybrid portfolios for multiple sponsors.
3. Inline Inspection with Digital Traceability
Inline particle inspection, container-closure analytics, and contextual alarm systems reduce detectability lag and allow batch disposition decisions earlier in the manufacturing window. For executives, this translates into lower batch rejection risk and fewer post-fill remediation cycles.
4. Modular and Distributed Facility Models
Modular and distributed fill-finish models are increasingly being adopted, supported by qualified local facilities operating under globally aligned GMP oversight. CDMO’s engages with and support such models through partner qualification, quality governance, and regulatory alignment rather than standalone infrastructure ownership.
Why This Transition Matters for Decision-Makers:
- It aligns sterile assurance with planned EMA/FDA audit expectations rather than reacting after findings.
- It reduces the lifecycle cost of compliance without lowering scientific or regulatory standards.
- It supports regional manufacturing to strengthen access pathways for vaccines, oncology injectables, biosimilars, and high-potency biologics.
- It provides supply chain resilience where traditional centralised plants cannot support time-to-patient or affordability thresholds.
How DRK Research Solutions Strengthens Sterile Injectable Manufacturing Programmes?
DRK Research Solutions supports sterile injectable drug product manufacturing by integrating drug product formulation, aseptic processing, validation, and global compliance under a unified CDMO framework. This ensures clinical continuity, inspection readiness, and scalable supply for high-value injectable portfolios.
Key Capabilities and Impact:
- Aseptic Formulation and Fill-Finish: Controlled environments, validated utilities, and process discipline protect product integrity from early development to commercial batches.
- GMP Manufacturing Through EU-Approved Partner Facilities: GMP-aligned manufacturing execution is conducted through EU-approved facilities located in Europe and Asia. These qualified contract manufacturing organisations operate under harmonised quality systems aligned with EU and US CGMP expectations, with DRK providing regulatory oversight, partner governance, and quality alignment.
- Support for Complex Molecules: Expertise includes drug product development and manufacturing support for biologics, niche products, high-potency formulations, and temperature-sensitive injectables, with a focus on formulation stability, aseptic processing, and regulatory compliance rather than API or discovery-stage activities.
- Regulatory-Ready Documentation: Each engagement includes eCTD supportive data, method validation, stability studies, and cleanroom qualification records that meet global submission expectations.
- Flexible Batch Configuration: Clinical, scale-out, and commercial batch options avoid vendor or process transitions, reducing risk and protecting programme timelines.
Through this integrated approach, DRK Research Solutions helps sponsors reduce operational uncertainty, maintain sterility assurance, and progress sterile injectable programmes toward market with greater predictability.
Conclusion
Sterile injectable manufacturing has become a decisive factor in ensuring product quality, patient safety, and global supply readiness. When planned early, it stabilises formulation performance, strengthens contamination control, and accelerates regulatory alignment. Pharma and biotech teams increasingly rely on CDMO partners who can execute with precision, transparency, and GMP reliability.
With validated systems, inspection-ready documentation, and drug product process control from development to commercial scale, DRK Research Solutions helps sponsors reduce risk, maintain sterility assurance, and achieve consistent market supply.
For sponsors evaluating sterile injectable programmes across development, clinical supply, and commercial launch, early alignment with an integrated, globally compliant CDMO model reduces risk, strengthens regulatory readiness, and supports sustainable access,.
Engage with DRK Research Solutions to assess how your injectable programme can progress with greater predictability, compliance, and global reach and connect with DRK Research Solution’s CDMO team to plan your next programme.
FAQs
1. What is sterile injectable manufacturing in pharmaceuticals?
Sterile injectable manufacturing is the production of parenteral drug products in controlled aseptic environments to prevent microbial contamination and ensure patient safety. It applies to vials, ampoules, prefilled syringes, and infusion products.
2. Why is sterile manufacturing essential for injectable products?
Injectables enter the body directly, so any contamination can create serious clinical risks. Proper sterile processes protect potency, maintain product safety, and support consistent performance for biologics, vaccines, and critical care medications.
3. What core regulations guide sterile injectable facilities?
Facilities follow FDA, EMA, and WHO CGMP expectations, along with sterility assurance requirements such as HEPA-controlled cleanrooms, media fill validation, environmental monitoring, and container closure integrity testing.
4. What are common challenges in sterile injectable manufacturing?
Key challenges include maintaining aseptic room conditions, contamination control, fill finish precision, and validation of equipment and operators. These issues increase during scale up if not managed through robust process control and documentation.
5. How do CDMOs support sterile injectable manufacturing needs?
CDMOs provide compliant facilities, trained personnel, validated processes, and regulatory-ready documentation. This helps reduce development risk, streamline technology transfer, and support clinical or commercial supply without disruption.
